"In their full power": Long-awaited comfort arrives in Attawapiskat

June 23, 2020
Featured image
The fruits of labour: the Sutherland-Kioke family, Robert, Michelle, Raelynn and baby Kiera, pose alongside Neepeeshowan staff Christine Roy, RM, and second attendant Jennifer Tookate with the new birth bed at Weeneebayko Area Health Authority Hospital, Attawapiskat, ON.
The birth of your child is a memory that stays with you forever. Nine months of carrying life and then when it is time, it happens: the incredible ceremony of the birth of this new spirit. In the lead up to that time, you take the best care of yourself that you can. You nest. You plan for a safe and comfy place to give birth to the new life coming your way. That is the least you would expect when giving birth at a hospital in Ontario. Up until recently, as I learned through my chat with midwife Christine Roy, this was not the case at the Weeneebayko Area Health Authority Hospital in Attawapiskat, Ontario.
By Tamara Cascagnette
Christine Roy, a French midwife with Abenaki roots, heads up Neepeeshowan Midwives. The practice is the only one on the James Bay coast in Attawapiskat, a little over 1200 kilometres north of the city of Toronto. If you Google the directions to Attawapiskat on your smartphone, the app will indicate that there is no way to get there. Of course, there is. The journey will take planes, trains and automobiles. It is a definite challenge to live in the north, as well as to run a midwifery practice in the remote fly-in community. In southern Ontario, we take for granted things that are a luxury in the north. For example, at the time of the interview, Christine was at her family home in Quebec, packing up quarts of berries to take back to Attawapiskat. Fresh, ripe, reasonably priced berries are easily accessible here in the south almost year-round. Up in the north, if you can get berries at all, they would be exorbitantly priced—close to ten dollars for six ounces.
The birthing bed at the Weeneebayko Area Health Authority Hospital, Attawapiskat, ceased working properly decades ago, stuck with the head of the bed below the lower two thirds of the unit—not comfortable in any situation, let alone when readying for the birth of a baby. When the bed did work, it took two people to make any adjustments to its positioning. Even with the donations gathered by Christine and Elder Dorothy Wynne, there was definitely not nearly enough to cover the cost of replacing the bed. A new unit costs about the same as a new, midsize car. The price increases by a few thousand dollars once you include the cost of shipping.
Prior to becoming a midwife, Christine worked as a nurse at the former hospital in Attawapiskat, James Bay General. The same bed had been there at that time. The year: 1988. “(The bed) was always horrible; always a frustration,” recounts Christine. An online search turned up beds similar to the one pictured below that were sold in the 1970s, making the bed in the obstetrics unit approximately 45 to 50 years old!
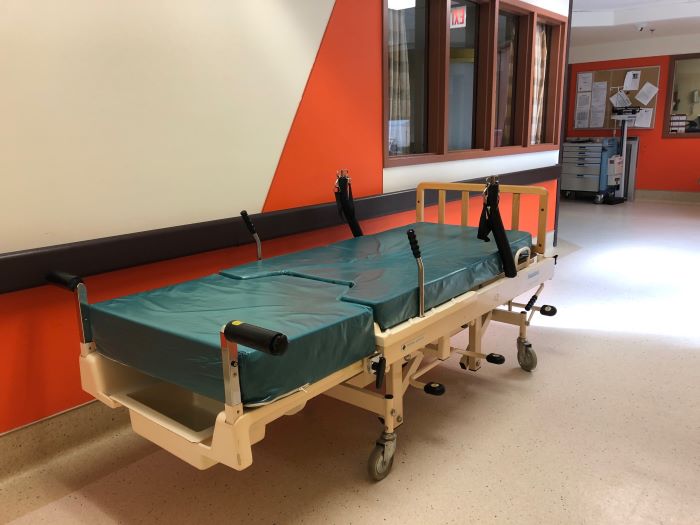
For four years, Christine hounded decision-makers for a new birthing bed for labouring clients. The response would be a definite “no,” or, further to her frustration, she would receive no response at all. Still, Christine and her team continued on in their work as midwives, assisting most clients to give birth “in their full power, standing up.” In their full power or not, labouring and giving birth takes a lot of energy. The client, she knew, needs to rest comfortably somewhere.
In February 2019, the Indigenous Midwifery Team at the Association of Ontario Midwives, along with a planning committee from agencies across the province, led the 2019 Indigenous Midwifery Summit (IM Summit) in Thunder Bay, Ontario. Initially planned as a small event to discuss the restoration of Indigenous Midwifery in northern Ontario, the gathering soon swelled to attract support and interest from Indigenous Political Territorial Organizations, Sioux Lookout First Nations Health Authority, both the Ministry of Health for Ontario and First Nations and Inuit Health Branch, as well as Indigenous community members and frontline workers. In the end, the event garnered the interest of almost 150 participants from Indigenous communities throughout the province, including presenters and planning committee members.
Because of her unique position and valuable experience providing midwifery care in the remote fly-in community, the IM Summit planning committee asked Christine to come to Thunder Bay to share about her work with the conference attendees. As she described both the challenges and the successes within her practice, her expertise and experience clearly demonstrated that midwives can successfully provide services in remote Indigenous communities. Christine recounted having to fight to keep the obstetrics services department open at the local hospital, as well as having to work with obsolete systems and equipment, both so old and lacking that they could not support the work of visiting specialists and patients in labour.
On day two of the Summit, Christine, spoke on a panel entitled, “Effects of Evacuation and the Barriers to ‘Rematriating’ Birth.” During the panel discussion, Christine conveyed the challenge of providing midwifery services to a mostly Cree community of 1,900, including emergency care to clients who arrive in preterm labour or with a placental abruption. At these times, Christine shared that she and her team and the nurses on staff are the emergency department. Emergencies like this are especially stressful while waiting for transport to an upper level hospital. Waiting on Ornge transportation services can take anywhere from hours to days, depending on weather conditions.
Adding to the stress was the broken bed.
Throughout the room at the Indigenous Midwifery Summit were changemakers, visionaries, Elders and spiritual leaders. The energy in the room was palpable. There was participation from each direction, and we were all there for the same reason: to envision bringing Midwifery home to Indigenous communities in the north.
They say that when things are supposed to happen, they will. The Creator puts those in our path who were needed to move things forward. The smoke that rose from the semaa (tobacco) in the seven pipes that were lifted at the opening of the Indigenous Midwifery Summit carried the prayers that were answered that day.
Following Christine’s panel, Ellen Blais, the Director of Indigenous Midwifery at the Association of Ontario Midwives, recognized those changemakers in the room. Always one to pull a team together for a cause, Ellen assembled representatives from the First Nations and Inuit Health Branch and the Ontario Ministry of Health to discuss what they could do to assist Christine in getting a new birthing bed at Weeneebayko Area Health Authority Hospital in Attawapiskat. Together, finally, they found a way to make it happen.
Everything fell into place. Funding was secured and arrangements were made for delivery of this vital equipment to the remote northern community. Christine shared, “I was so afraid that something would go wrong that I didn’t even tell anyone until the week the bed was arriving.” Fortunately, all of her fears were put to rest with the arrival of the new bed.
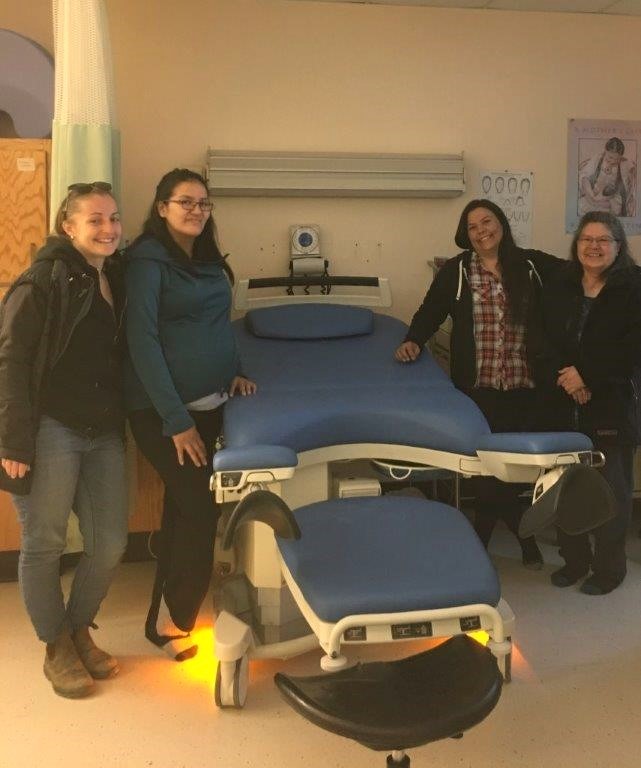
This new birth bed has since been put to use by several members of the community. The bed is equipped with many great features: a squat bar, adjustable leg supports, soft lights and an over-mattress that can be put into place postpartum. Most importantly, there are options for positioning that can be changed to suit the needs of the client, as well as to provide ease of access for the midwife.
Christine’s dogged determination to get a sorely needed birthing bed into the Attawapiskat hospital paid off. It was a proud moment for Christine and those who supported her efforts to have the bed funded and in place to provide comfort and support to those giving birth in this remote Indigenous community.

